Overview
Managing a cancer diagnosis is a team effort, and everyone has their role — including you. However, along with learning about your cancer and treatments and planning for potential side effects, “regular” life must still go on. You simply can’t be expected to shoulder everything on your own. That is where supportive care comes in.
Being proactive allows you to be an informed partner in your care and side effect management.
Report side effects as soon as they occur. Don’t wait until your next appointment. Some people try to muscle through because they are afraid they will be taken off their drug or the dosage will be reduced, preventing them from treating their cancer as aggressively as originally intended. Others hesitate to “bother” their health care provider. The days of not being able to talk to the people in charge of your medical care are gone. You and your health care team must work together. Ask all your questions, and answer theirs. Share concerns before and during treatment, such as what side effects to expect and how to minimize them before treatment begins.
Build a Foundation
Give yourself a solid foundation by starting with the following.
Get a second opinion. A specialist or cancer center that has extensive experience treating your type of cancer can confirm your treatment plan or offer more information to consider. You deserve to learn all your options, especially if you have a rare diagnosis.
Secure your caregiver. Everyone needs at least one support person to help them navigate a cancer diagnosis. Your caregiver will be integral to nearly every part of your journey.
Set up your health care portal. Most health care facilities offer an online portal as a primary means of communication. Often available as a phone app, it is an easy way to ask non-urgent questions, review test results and more. The information on the portal is a permanent part of your health care record.
Get names and contact information. Ask for the names of your main supportive care contacts and the best ways to reach them, such as through the portal, app, by phone or by text. Introduce your caregiver to your key contacts and have them fill out the appropriate HIPAA forms so they can communicate with the team, refill prescriptions, etc.
Ask about telehealth. Find out if telehealth appointments are available when in-person visits aren’t necessary.
Your Supportive Care Team
Because cancer affects every part of your life, it can often feel like you’re caught in a storm. The following services can offer an umbrella of support, making your life easier (see Figure 1).

Case management. A case manager coordinates your care from diagnosis through treatment and recovery, often working with the insurance company and providing resources to help manage the financial burden of cancer care.
Palliative care. This improves the quality of life and helps reduce pain in people who have a serious or life-threatening disease, such as cancer, from diagnosis until the end of life. The goal is to prevent or treat disease symptoms and treatment side effects. It may include treatments and addresses the related psychological, social and spiritual problems, and family and caregiver support.
Community & resources. Your cancer community includes advocacy and support groups, your caregiver, family, friends and neighbors. Talking with someone who has been in your shoes can be very healing. Sometimes the biggest hurdle is accepting help. The people around you will likely want to help, they just need to know what you need most. Be specific when they ask what they can do, such as bringing meals or taking you to an appointment.
Your Health Care Team
You may see any of the following medical professionals.
Physicians:
Cardiologist
Hospitalist
Interventional radiologist
Medical oncologist
Physician who specializes in your type of cancer
Radiologist
Surgical oncologist
Nurses:
Infusion therapy nurse
Nurse practitioner
Palliative care nurse
Patient or nurse navigator
Registered nurse
Health professionals:
Case manager
Chaplain
Nutritionist
Occupational therapist
Pain specialist
Patient navigator
Pharmacist
Physical therapist
Psychologist
Respiratory therapist
Sex therapist
Social worker
Speech therapist
Potentially Severe Side Effects
Treating cancer requires powerful and often life-saving therapies. Unfortunately, the side effects from these aggressive treatments, known as adverse events, can be serious. In some cases, they can even be life threatening. Before you begin treatment, talk with your health care team about the adverse events that may happen with your type of treatment, what to do if they occur and when they require immediate action. Then, do your part by following medical instructions, staying in tune with your body and communicating with your health care team.
Being honest with your health care team about adverse events as soon as they occur is really important. They can often be reversed if they are treated early. However, if you allow them to progress, symptom management becomes more complicated and may interfere with treatment. Although you may worry that you will be hospitalized or your treatment will be stopped, keeping these side effects a secret won’t help. Things will only get worse — not better. Your team is dedicated to helping you and, to do so, they rely on your honesty.
The adverse events that you experience, how severe they are, how you react and how to manage them will depend on many factors: your diagnosis, your risk factors, allergies, other health conditions, age and more. Make sure you understand as much as you can about your diagnosis, the medications in your treatment plan and your responsibilities as your own advocate before you begin treatment.
The following types of potentially severe side effects, in alphabetical order, may occur.
- Cytokine release syndrome (CRS) can occur if immune cells affected by treatment rapidly release large amounts of cytokines into the bloodstream. This process can send the immune system into overdrive, leading to CRS. Symptoms may include headache, fever, nausea, rash, low blood pressure, rapid heartbeat and difficulty breathing. See more here.
- Immune effector cell-associated neurotoxicity syndrome (ICANS) is a clinical and neuropsychiatric syndrome that can occur in the days to weeks following treatment with certain types of immunotherapy, especially immune effector cell (IEC) and T-cell engaging therapies. ICANS affects a person’s nervous system. It is the second most common side effect of CAR T-cell therapy, often following cytokine release syndrome.
- Immune-related adverse events (irAEs) may occur with certain immunotherapy drugs if the immune system becomes overstimulated by treatment and causes inflammation in one or more organ or system in the body. Some irAEs can develop rapidly, becoming severe and even life-threatening without immediate medical attention. See more here.
- Infections can occur when harmful organisms, such as bacteria, fungi and/or viruses, invade your body and multiply, resulting in disease, illness or damage to your organs and tissues. Normally, your immune system destroys these germs before they can cause harm. But, because cancer and its treatments weaken the immune system (sometimes resulting in a low white blood cell count known as neutropenia/leukopenia), your immune system often cannot destroy the harmful organisms fast enough. See more here.
- Infusion-related reactions most frequently occur with treatment given intravenously (IV) through a vein in your arm, usually soon after exposure to the drug. Reactions are generally mild, such as itching, rash or fever. More serious symptoms, such as shaking, chills, low blood pressure, dizziness, breathing difficulties or irregular heartbeat, can be serious or even fatal without medical intervention. See more here.
- Tumor lysis syndrome (TLS) may occur after the treatment of a fast-growing cancer, especially certain blood cancers. Symptoms may include vomiting, diarrhea, muscle cramps or twitches, neuropathy and decreased urination. TLS can potentially cause damage to the kidneys, heart, liver or other organs. See more here.
Common Physical Side Effects
Most cancer treatments have side effects, and many people dread them as much as the cancer itself. Being proactive and learning what to expect will help you create a plan to prevent side effects from affecting your quality of life too drastically. Talk with your health care provider before treatment to learn about the side effects below and any others that may apply to you. And, as you proceed through treatment, take the approach of “see something, say something” and immediately contact your health care provider about any new symptoms.
Although most cancer treatments have side effects, it may comfort you to know that advances in research have made it possible to minimize and even prevent some of them. The key is communication.
As you talk about your treatment options with your health care provider, discuss the potential side effects of each option so you consider them based on your expectations for your quality of life. Ask how to recognize symptoms and when to expect them. Make sure you know what to do if a side effect occurs and when to seek medical attention.
Continue to update your health care team between your follow-up appointments about your symptoms, including when they occur, how they make you feel and whether anything relieves them. You can download a free tracker at PatientResource.com/Tracker to help you remember the details. Addressing side effects early is important because when you feel better, you will be more likely to stay on your treatment plan.
Manage Your Feelings and Mental Health
You know yourself best. If during your cancer journey, you experience anxiety, depression, distress, anger, fear and other emotions, don’t be afraid to share them with your health care provider. If you don’t address these feelings, they can interrupt your treatment plan, causing you to miss medical and therapy appointments. They can even cause physical health problems, such as suppressing the immune system, decreasing the body’s ability to fight infection and increasing the risk for serious illness like heart disease and stroke.
Talking with a member of your health care team as soon as symptoms start – or even if something just doesn’t feel right – is a great way to take charge of your mental health. Often cancer and mental health problems will present with the same symptoms, making it difficult to distinguish between them, including fatigue, nausea, decreased appetite, cognitive (thinking) changes and sleep problems.
Following are some emotions you may experience and suggestions for ways to feel better.
Anxiety about your diagnosis, treatment, recurrence or long-term survival is common. Waiting for test results during follow-up appointments and scans can raise anxiety levels because those test results often give you life-altering information, such as whether the cancer is responding to treatment. Referred to as scanxiety, cancer survivors, caregivers, friends and loved ones often face it.
Depression is characterized as ongoing sadness and/or loss of interest in activities. The following are signs of depression:
- Prolonged feelings of sadness and/or anxiety
- No longer being interested in activities you once enjoyed
- Difficulty concentrating or doing daily tasks
- Irritability
- Low energy levels
- Changes in sleep or eating habits
- Increased use of drugs or alcohol
- Have thoughts of harming yourself or suicide
Anxiety disorders are different than everyday worries. They may lead to intrusive thoughts that result in persistent anxiety. Symptoms include excessive worry and nervousness, mood swings and physical symptoms such as palpitations, sweating and shortness of breath. Treating an anxiety disorder may improve your ability to cope with your diagnosis.
Post-traumatic stress (PTS) and post-traumatic stress disorder (PTSD) reactions may include repeated frightening thoughts, being distracted or overexcited, having trouble sleeping and/or feeling detached from yourself or reality. PTS can occur at any point during the cancer journey. In some cases, PTS can lead to PTSD, which is often more severe and can last longer than PTS. Some typical symptoms may include avoiding medical appointments, blaming yourself for the illness, experiencing survivor’s guilt, and having difficulty sleeping and/or concentrating.
Distress is most likely to occur during diagnosis, when a new symptom arises or the cancer has returned. It can also happen while waiting for treatment to start, when symptoms worsen or when another health problem is caused by treatment.
Fear is a common reaction to finding out you have cancer and facing treatment. Fears include not knowing what to expect, pain during or after treatment, inability to do daily activities while in treatment, a change in appearance (hair loss or scars), fertility issues and sexuality challenges. One of the ways to combat fear is to learn as much as you can about your cancer and your treatment. Talk to others going through similar treatment. Support groups, both in person and online, may be helpful.
Loneliness is a feeling of being alone and isolated from others. You may feel alienated or that no one else understands what you’re going through. It may help to talk to people who have the same type of cancer as you. Contact a support group, confide in a close friend or reach out to a member of your faith or spiritual community.
Grief is the feeling of distress or sorrow due to the loss of something. It is normal to grieve the loss of your health, your appearance or your ideas of what your future would be without cancer. Allow yourself to feel a full range of emotions. Ask your friends and family for support.
Recognizing Roadblocks
Many people are reluctant to, or face barriers to, receiving mental health services. Or they may not recognize their symptoms as indicators of emotional distress. Social norms and gender roles may prevent them from exploring resources, and the risks of rejection and stigma may stifle the desire to ask for help. Can you relate to those feelings or are you experiencing any of the following?
- Struggling to acknowledge the emotional impact of the diagnosis and, instead, coping by stuffing down your feelings.
- Having difficulty admitting you need help, asking for help or accessing help.
- Choosing to avoid facing painful emotions.
- Not wanting to talk about cancer at all to distract yourself from thinking about it.
- Having trouble expressing difficult emotions especially because you don’t want to burden friends or family.
- Fearing that sharing your feelings will cause friends and family to pull away from your relationship.
- Not believing that talking about feelings can even be helpful, regardless of whether it is to other survivors or to mental health professionals.
- Wanting to focus on “just getting through treatment.”
- Having physical symptoms that you assume are only physical side effects.
It may comfort you to know that all of these feelings are valid, and many people who have sought mental and emotional support during or after cancer treatment have found it helped. Some say it felt like a weight was lifted from their shoulders, and it made it easier to manage their everyday anxiety.
Let your health care team know as soon as you experience any symptoms. Don’t be embarrassed to speak up and share your feelings. The sooner your team knows, the sooner they can help.
Getting the Help You Need
How you have dealt with a serious life crisis in the past might set the stage for how to approach this medical crisis. If your methods worked well, they are worth repeating. If they did not, don’t try to use them for this situation.
Try these methods for improving your mental health:
- Increase your self-awareness. Find out what triggers you, such as certain people, calendar dates, treatment ending, the change of seasons, etc.
- Treat feelings as a visitor. Don’t fight them; acknowledge them and move forward.
- Treat yourself with compassion. Notice when you are in distress and show yourself kindness. Remind yourself that it is okay to feel distress, and remember that being imperfect is part of being human.
- Pay attention to the present. Try practicing mindfulness, which is the practice of noting the present moment or an emotion for what it is without feeling the need to change how you’re feeing or push the emotion away.
- Take good care of yourself.
Many cancer centers have counselors to help coach you, but you may need to ask for them. In general, a supportive care team includes social workers who can help you cope with life challenges, psychologists who are experts in how people think, feel and behave and psychiatrists who are licensed medical doctors specializing in mental health. They are trained to help people with cancer from diagnosis and for as long as needed.
Support groups are available online, through social media, by phone and in person. Some advocacy groups can connect you with helpful resources and may be able to connect you with another survivor who has a similar diagnosis. Peer-to-peer counseling, especially talking to someone else who may be at the same stage in life (just getting out of school, just married, a new parent or newly retired, for example), can be extremely helpful. Most survivors will gladly offer suggestions on what works for them.
Mental health issues don’t always stop after treatment ends. Emotions can come up months or even years later. Take the suggestions for managing your mental health to heart because it is as important as your physical health. Allow yourself to express your feelings freely. Being emotionally healthy will help you better cope with cancer-related issues. It’s okay to not be okay. The important thing to remember is that you are not alone.
If you or a loved one is experiencing a mental health crisis, dial 988 to talk to a trained mental health professional. It is free, confidential and always available.
| Treatment Type | Side Effect* |
| Chemotherapy | Anemia, appetite loss, blood disorders, bone loss, cardiotoxicity (heart problems), cognitive dysfunction (memory problems), constipation, diarrhea, fatigue, fertility issues, hair loss, mouth sores, nausea and vomiting, nervous system effects, neutropenia, pain, skin and nail changes, weight changes |
| Hormone Therapy | Cognitive dysfunction (memory problems); deteriorating bone health; fatigue; gastrointestinal symptoms; higher risk for other health issues including blood clots, cataracts, heart attacks and strokes; hot flashes and night sweats; infertility; mood changes; sexual health concerns; vaginal and menstruation changes (in women) |
| Immunotherapy | Anemia, bone marrow suppression, breathing problems, constipation, cough, cytokine release syndrome (CRS), diarrhea, eye problems, fatigue, fertility issues, fever, gastrointestinal problems, immune effector cell-associated neurotoxicity syndrome (ICANS), immune-related adverse events (irAEs), infections, infusion reactions, kidney problems, lower blood counts, muscle and joint pain, neuropathy, skin reactions |
| Radiation Therapy | The location of the tissues that are being radiated greatly influences what side effects may occur with the exception of fatigue, which happens for most people. Bone loss, cardiotoxicity (heart problems), cough, diarrhea, difficulty swallowing, dry mouth, extreme fatigue, fever, hair loss (in the area of the body being treated), headache, incontinence, lymphedema, mouth sores, nausea and vomiting (if abdomen is radiated), rectal bleeding, sexual and fertility problems (if pelvis is radiated), shortness of breath (if chest is radiated), skin sensitivity, tooth decay (if the head or neck is radiated). |
| Stem cell Transplantation | Anemia, appetite loss, blood clots (thrombocytopenia), diarrhea, fatigue, Graft-versus-Host Disease, hair loss, infections, mouth sores, nausea and vomiting, taste changes, weight loss |
| Surgery | Body image changes, bruising, constipation, drainage, fertility issues, limited mobility, lymphedema, numbness, pain, slow digestion, swelling |
| Targeted Therapy | Acne-like rash, blood clots (thrombocytopenia), cardiotoxicity (heart problems), constipation, diarrhea, dry or itchy skin, fatigue, flu-like syndrome, increased risk of infection, mouth sores, nausea and vomiting, neutropenia |
Understanding how targeted therapy works
Targeted therapy is a personalized systemic drug strategy that uses the results from genomic and biomarker testing to select a drug therapy that targets specific genes, receptors, proteins, mutations, abnormalities or other factors that are involved in the development and support of the tumor. They attack cancer in different ways.
Small molecule drugs are able to get inside a cell and target its internal components. These drugs can target the cancer’s gene expression, enzymes that affect the tumor, or certain proteins.
Angiogenesis inhibitors block new blood vessel growth that feeds tumor cells. Tumors need a blood supply to survive and grow. Without it, the tumor cells cannot survive.
Monoclonal antibodies (mAbs) are laboratory-made antibodies designed to target specific tumor antigens, which are substances on tumor cells that cause an immune response. They can flag targeted cancer cells for destruction, block growth signals and receptors, and deliver other therapeutic agents directly to targeted cancer cells.
Different types of mAbs include the following:
Naked mAbs work by themselves. No drugs or radioactive particles are attached.
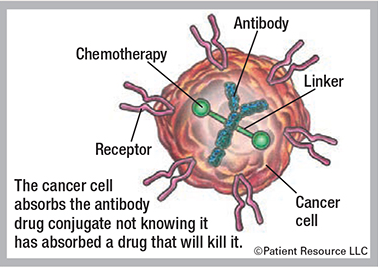
Conjugated mAbs have a chemotherapy drug or a radioactive particle attached to them. They deliver treatment to the cancer cells. Types include radiolabeled antibodies, which deliver radioactive particles, and antibody-drug conjugates, which deliver a chemotherapy drug (see Figure 1).
They attach to specific receptors or proteins on the cancer cell, get swallowed by the tumor cell and break down inside the cell, releasing the toxin and causing cell death.
Bispecific mAbs are made up of two different mAbs (see Figure 2). They can be used for engaging and activating immune cells, such as T-cells, to attack a tumor, block dual signaling pathways, block immune checkpoints or form a way to replace a missing functional protein.