Male Breast Cancer
Overview
Feeling overwhelmed after receiving a cancer diagnosis is normal, especially when it is a cancer you may not have realized you could even have. As you learn medical terms, meet new health care professionals and make treatment decisions, be patient with yourself. It is a lot of information to digest, but it may be easier if you learn as much as you can about your diagnosis and surround yourself with support.
Breast cancer basics
Breast cancer in men is not common but does occur. It can develop in men at any age, with the average age at diagnosis between 65 and 70 years.
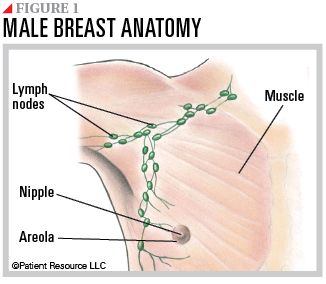
The breasts are made up of connective, fatty and fibrous tissues (see Figure 1). Though a lump may seem easier for men to feel because they typically have less breast tissue than women, they may ignore it or not report breast changes to their doctor because they may not realize they are at risk. They also do not obtain screening mammograms. As a result, male breast cancer may be diagnosed at a late stage. This delay in diagnosis can allow the cancer to spread to lymph nodes under the arm or around the collarbone, even before the original tumor in the breast tissue is large enough to be felt.
When genes in normal breast cells mutate and cause the cells to multiply uncontrollably, they form a disorganized mass of abnormal cells called a tumor. Some tumors are benign. Some are malignant, such as breast cancer. Cancer cells can penetrate and damage nearby organs and tissues. They can also break away and spread to other parts of the body through the bloodstream or lymphatic system, a process known as metastasis. When this occurs, the cancer cells are still considered breast cancer, regardless of where it spreads.
Breast cancer is not always felt as a lump. Sometimes it is detected as a bloody nipple discharge or on a mammogram or breast ultrasound.
The following types of breast cancer are commonly diagnosed in men:
• Ductal carcinoma in situ (DCIS) involves abnormal cells in the lining of a duct.
• Infiltrating ductal carcinoma , the most common, occurs when cancer spreads beyond the cells lining ducts in the breast.
• Inflammatory breast cancer has spread to the skin of the breast. The breast looks red and swollen and feels warm because the cancer cells block the lymph vessels in the skin. The skin of the breast may appear dimpled, like an orange peel. There may not be any lumps in the breast that can be felt.
• Invasive breast cancer spreads beyond the ductal or lobular structures into surrounding fatty and fibrous breast tissue and other organs.
• Paget’s disease of the nipple involves a tumor that has grown from ducts beneath the nipple onto the surface of the nipple.
Explaining Genomics & Genetics
Genomics and genetics just sound complicated, right? They don’t have to be. The following may help you understand what they are and why your doctor uses them to determine your diagnosis and decide how aggressively to approach treatment. As always, if anything isn’t clear or if you have more questions, ask your doctor for more information.
Genetics and genomics are not the same thing. Germline genetics is the study of genes and the passing of genetic information and traits from parents to offspring (heredity). Tumor genomics refers to the study of the genes and DNA within a person’s tumor. Germline genetic testing may be performed before or after someone is diagnosed with cancer, to determine whether a cancer-causing gene was inherited.
Tumor genomic testing is done to identify specific mutations within the tumor, which may help determine whether there are specific or targeted treatments available. In breast cancer, it is routine to test for the hormone-related biomarkers estrogen receptor ( ER ) and progesterone receptor ( PR ) as well as human epidermal growth factor receptor-2 ( HER2 ), which encodes a growth-promoting protein. HER2 + breast cancer results in overproduction of the HER2 growth factor.
The BReast CAncer 1 gene (BRAC1) and BReast CAncer 2 gene ( BRAC2 ) are the most common mutations in breast cancer. These genes produce proteins that help repair damaged DNA. Everyone has two copies of each of these genes — one copy inherited from each parent. BRCA1 and BRCA2 are sometimes called tumor suppressor genes because when they have certain changes, called harmful (or pathogenic) variants (or mutations), cancer can develop.
When categorizing mutations, the two main types are acquired (genetic damage that occurs during a person’s lifetime) and germline (a genetic mutation that comes from the sperm or egg of the parents that is passed on to the child at conception.
Most cancers are caused by acquired mutations. Germline mutations are less common, and genetic testing is typically done to detect these mutations to determine future cancer risk, especially if there is a history of certain cancers in the family. However, inheriting a germline mutation doesn’t mean a person will automatically develop cancer; it only means the risk is increased.
Mutations are common and don’t automatically cause cancer, but when mutations cause cells to produce too many abnormal genes or proteins, they can interrupt normal bodily functions and become cancerous.



