Head & Neck Cancer
Treatment Planning
Research is expanding the type of head and neck cancer treatments available. Scientists are looking to find more effective therapies, including drugs, drug combinations, surgical techniques and types of radiation therapy. Improving side effect management to help improve patients’ quality of life is also a goal.
Your treatment plan will be based on many factors: whether you are newly diagnosed or are experiencing a recurrence; the presence of symptoms; your overall health; the aggressiveness of the cancer; and your goals of treatment, which may include curing the cancer, controlling tumor growth and pain, and improving your quality of life.
Flexibility and patience will become very important. The treatment plan you start with may change if test results or symptoms indicate the need. Your doctor will monitor you regularly, and you will be responsible for communicating with your health care team and keeping follow-up appointments.
Your doctor may ask you about your smoking status to determine the potential effectiveness of radiation therapy and surgical treatments. Smoking is known to reduce treatment effectiveness and is also associated with an increased risk of second cancers.
Treatment Options
Treatments can be used alone or in combination and at different times. First-line therapy is the first treatment used. Second-line therapy is given when the first-line therapy does not work or is no longer effective. Standard of care refers to the most widely recommended treatments for the type and stage of cancer you have.
Local treatments are directed at a specific organ or a limited area of the body and include surgery and radiation therapy. Systemic treatments, which are typically drug therapies, travel throughout the body.
Your treatment options may include the following.
Surgery is used to remove a solid tumor. It may offer the best chance of controlling the disease and keeping it from spreading, especially for people with early-stage disease. Surgery may be used to stage and treat the cancer or to relieve or prevent symptoms that might otherwise occur later. Many types of surgery are available. A neck dissection, which is the removal of lymph nodes and surrounding tissue from the neck, is a common procedure that may be used. Surgery may also accompany other treatment types.
Reconstructive surgery may be an option to restore appearance or functionality (see Reconstruction & Rehabilitation).
Radiation therapy uses high-energy radiation to destroy cancer cells and shrink tumors. Some people with localized disease or bone pain that does not lessen with chemotherapy may receive it to specific parts of the body.
External-beam radiation therapy (EBRT) is the most common type of radiation therapy used to treat many types of head and neck cancer. It is delivered from a machine. Different types of EBRT include proton therapy, three-dimensional conformal radiation therapy (3D-CRT), intensity-modulated radiation therapy (IMRT), hyperfractionated therapy and stereotactic radiosurgery.
Radioactive iodine therapy involves giving radioactive iodine (I-131) in liquid or pill form to treat some forms of thyroid cancer. It may be used after surgery in patients with thyroid cancer who are at increased risk of recurrence. The radioactive iodine will concentrate in any remaining thyroid tissue, and the radiation will kill the cancer cells.
Drug therapy may include chemotherapy, hormone therapy, immunotherapy or targeted therapy.
Chemotherapy is typically used only in patients with advanced head and neck cancers. It may be given alone or in combination with other forms of treatment. It may be given intravenously (IV) through a small tube inserted into a vein or port, or taken orally as a pill. Most patients with early-stage head and neck cancers do not receive chemotherapy.
Hormone therapy is a part of treatment to supplement the hormone the thyroid gland makes if the thyroid is partially or fully removed. It may also be used to slow down the growth of remaining differentiated cancer cells. It is typically given orally as a pill that is taken daily.
Immunotherapy helps the body’s own immune system recognize and destroy cancer cells. It may be used as first-line therapy for metastatic, recurrent or unresectable (inoperable) head and neck cancers. It may be used when the cancer progresses during or after platinum-based chemotherapy. The main type of immunotherapy approved for head and neck cancers is immune checkpoint inhibitors, which prevent the immune response from slowing down so that immune cells continue fighting cancer. It may be given intravenously (IV) through a vein or a port or as an injection.
Some immunotherapies are approved as tumor-agnostic treatment, which means they are approved to treat any type of cancer that has the molecular alterations known as microsatellite instability-high (MSI-H), deficient mismatch repair (dMMR) or tumor mutational burden-high (TMB-H).
Targeted therapy uses drugs or other substances to identify and attack specific cancer cells. Targeted therapy is designed to affect only cancer cells. Some of these drugs are oral medications given in pill form, and others are given by IV. Some may be given alone or in combination with other drug therapies.
When given for head and neck cancers, these drugs target specific genes, such as BRAF, RET and NTRK, or proteins and growth factors, including VEGF, EGFR and MEK. This therapy may be used with or without chemotherapy and after surgery for advanced stage head and neck cancers.
Chemoradiation, also called chemoradiotherapy, combines chemotherapy with radiation therapy. It makes cancer cells more sensitive to radiation, making it easier for the radiation to kill them.
Watchful waiting, sometimes known as active surveillance, may be recommended for tumors that appear to be growing very slowly. Delaying treatment postpones potential treatment side effects for as long as possible while the doctor closely monitors for signs the cancer has progressed or returned.
Clinical trials are medical research studies that may offer access to leading-edge treatments not yet widely available. They may be an option at any stage, even as a first-line treatment (see Clinical Trials). Ask your doctor whether you should consider a clinical trial.
Some Head and Neck Cancer Drugs
These therapies may be used alone or in combination.
| Some head and neck cancer drugs |
| bleomycin sulfate (Blenoxane) |
| cabozantinib (Cabometyx, Cometriq) |
| cetuximab (Erbitux) |
| cisplatin (Platinol) |
| dabrafenib (Tafinlar) and trametinib (Mekinist) |
| docetaxel (Taxotere) |
| doxorubicin hydrochloride (Adriamycin) |
| entrectinib (Rozlytrek) |
| hydroxyurea (Hydrea) |
| larotrectinib (Vitrakvi) |
| lenvatinib (Lenvima) |
| methotrexate sodium (Methotrexate LPF) |
| nivolumab (Opdivo) |
| pembrolizumab (Keytruda) |
| selpercatinib (Retevmo) |
| sorafenib (Nexavar) |
| toripalimab-tpzi (Loqtorzi) |
| vandetanib (Caprelsa) |
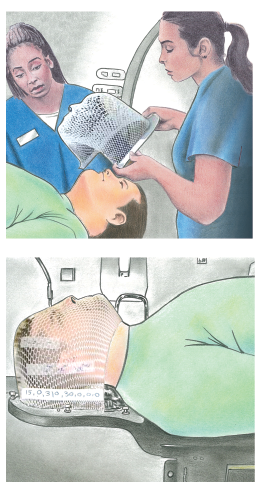
Thermoplastic Mask
Mask ensures accurate delivery of radiation beams
Radiation beams must target the same spot every time for radiation therapy to be most effective. In most cases, semi-permanent marks or permanent tattoos are placed on your skin to indicate the exact location the radiation beams must hit to reach the tumor. To ensure your safety, you must be in the same position for every treatment. Body molds or other immobilizing devices, such as a special mesh head mask called a thermoplastic mask, may be necessary.
The mask is created from a mold of your face and head, and it is a tight fit. Wearing it and being unable to move can cause anxiety, especially if you are claustrophobic. Your treatment team will help make you as comfortable as possible, so tell them if you feel anxious. Your doctor may prescribe medication to help you relax.



